Connecting with patients from afar.
Simplifying data analysis and remote intervention for nurses.
The brief.
Respirix is a biomedical company that produces the Cardiospire, a device that records 6 different biometrics at once from the comfort of the patient’s home. Not only does the Cardiospire record heart rate, temperature, blood pressure, and blood oxygen saturation, it has the ability to record lung sounds and functions using novel technology pioneered by Respirix. This positions Respirix as the sole provider of proactive cardiopulmonary health monitoring.
Not only does Respirix need to engineer the Cardiospire and develop an app for patients, they also need to create a platform for health providers to access and assess the patient data, as well as intervene from afar. My team and I were tasked to build the practitioner portal from scratch.
Duration.
3-week sprint
Team.
Me
Paige Baxter
Victoria Du
Tools.
Figma
Whimsical
Method.
Business analysis
Task analysis
Competitive and comparative analyses
User interviews
Affinity mapping
Collaborative design studio
Wireframing
Prototyping
Usability testing
THE PROBLEM
No visuals, no alerts, no chat, no portal.
Users need a way to analyze, prioritize, and intervene.
The core problem is quite simple: there is no platform for nurses to view the data collected from the Cardiospire. On top of that, from the research that we performed, not only do nurses need to have a comprehensive, consistent, and current snapshot of all patient details, they must also have a way to contact and intervene with the patient. Additionally, due to the user’s high volume of assigned patients, there is no current way to alert the user of a worsening trend that needs to be tended to.
We discovered that nurses need to have comprehensive patient data that is the same across all platforms, and that the UI of the practitioner portal must be easy to learn and navigate. Most medical professionals are already using existing electronic health record applications that are cluttered, overwhelming, and unintuitive. In essence, our target user is lacking an intuitive and comprehensive way to analyze patient data, receive automated alerts, and intervene with the patient from afar.
THE SOLUTION
Focus on the heart of it.
Determine and design core features for the first MVP.
Initially, our team was overwhelmed by the number of possible features that this product could have. It was clear, due to the tabula rasa nature of the project, that we really needed to focus solely on honing on the most important features for our first-iteration MVP.
After some research synthesis, we believed that providing an intuitive way of reviewing patients’ self-collected data, receiving automated notifications, and remotely intervening with patients via video would effectively solve the 3 most pressing needs of our busy target user. Not only that, but the program must be encrypted and instantaneously sync with their hospital’s EHR. On top of all these features, our product must be extremely easy to use as our target users range widely in tech literacy.
Solution objective.
1. Easy-to-decipher data visualization.
2. Automated alerts and notifications.
3. Constant reciprocal communication with EHRs.
4. Virtual visits and in-app messaging.
How we approached it.
Scoping the playing field.
Before we went to potential users for their input, we performed competitive and comparative analysis on a number of leading patient tracking portals like Healthsnap and Tactio. Performing these analyses gave us inspiration for how to approach certain features and how to interface them. They also shed light onto UX practices to avoid incorporating into our design. Specifically, we learned that most, if not all apps, included: a sort and filter feature, a notification system for worsening trends, in-app patient messaging, and long term chronic care management. This helped inform what features to include in our own design and how to implement them.
Determining primary needs straight from the source.
In order to provide a platform that users would find comprehensive and usable, we had to uncover what exactly our users needed to effectively monitor and intervene with patients from afar. Interviewing real medical professionals gave us valuable qualitative information that informed our MVP. We gained from these interviews the daily challenges and pressing needs of cardiopulmonary nurses in outpatient scenarios. Collecting these testimonials from 8 different medical professionals gave us enough diversity to tease out the common trends and unique perspectives, as explained below.
Revealing the patterns.
Once the interviews were complete, we had a high volume of qualitative data to process. By affinity mapping, we were able to group the insights into broader trends and categories. This helped us distinguish unique personal quirks from common sentiments and needs. From these findings, we created our persona, the Communicative Caretaker. Our target user acts as a liaison between patient and doctor, and needs to have a comprehensive snapshot and history of the patient’s health at all times. They are extremely busy and need to be able to understand their patients data quickly and easily. Creating the persona helped us make important design decisions about which features to include and how.
The moment of truth.
After we designed our first wireframe based off our research findings, we performed usability tests with our interview subjects to validate our design decision and reveal areas for improvement. The tests revealed that while our initial design was overall complete and intuitive, there were some minor changes to be made, namely: 1) the patients were missing helpful data like medication route and dosage, and 2) the alert notification classification was a little to broad and vague. To rectify these weak spots, we added more detailed information to the patient’s info page, and we created a tiered classification system that made better use of color and shape to distinguish severity.
Deliverables.
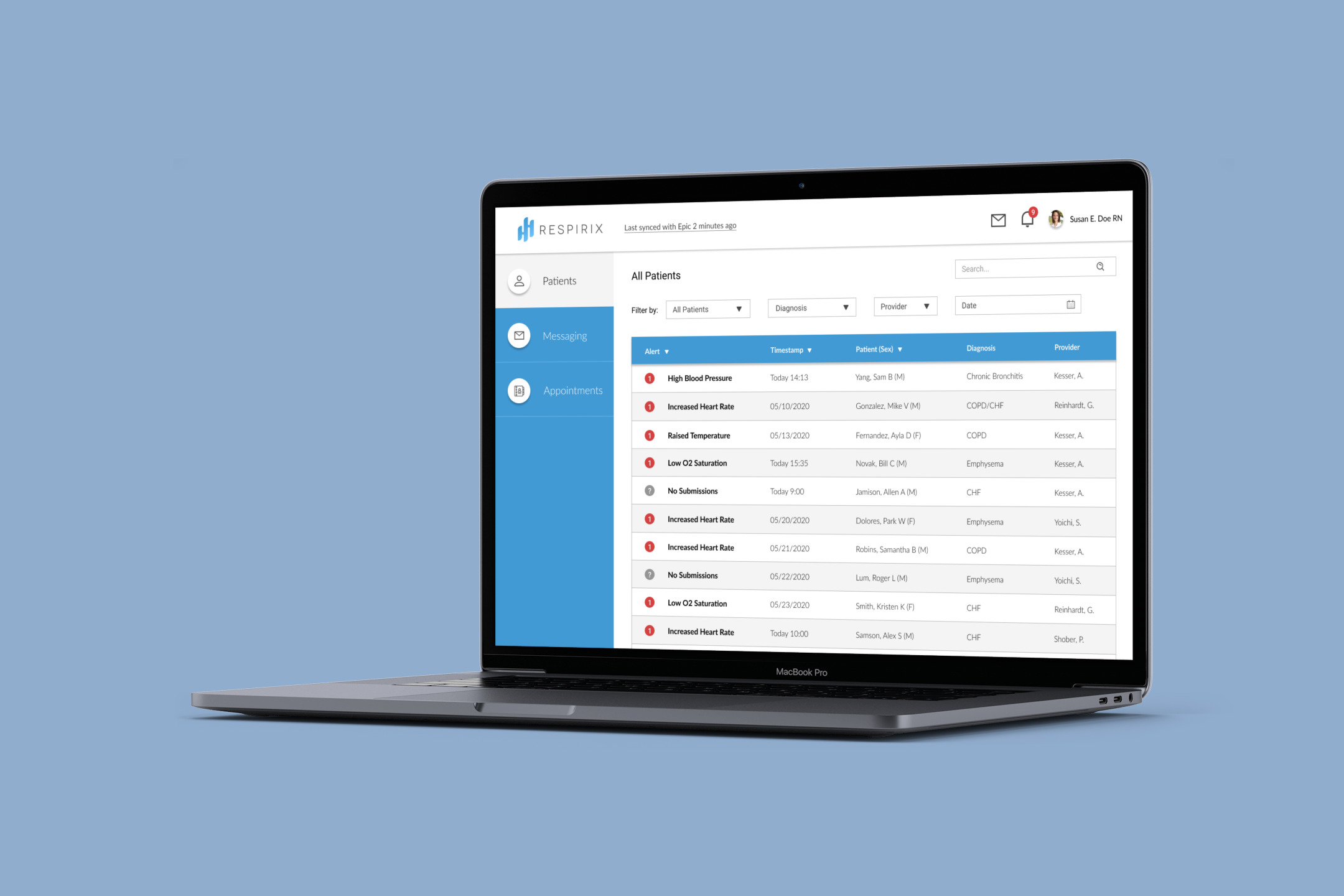
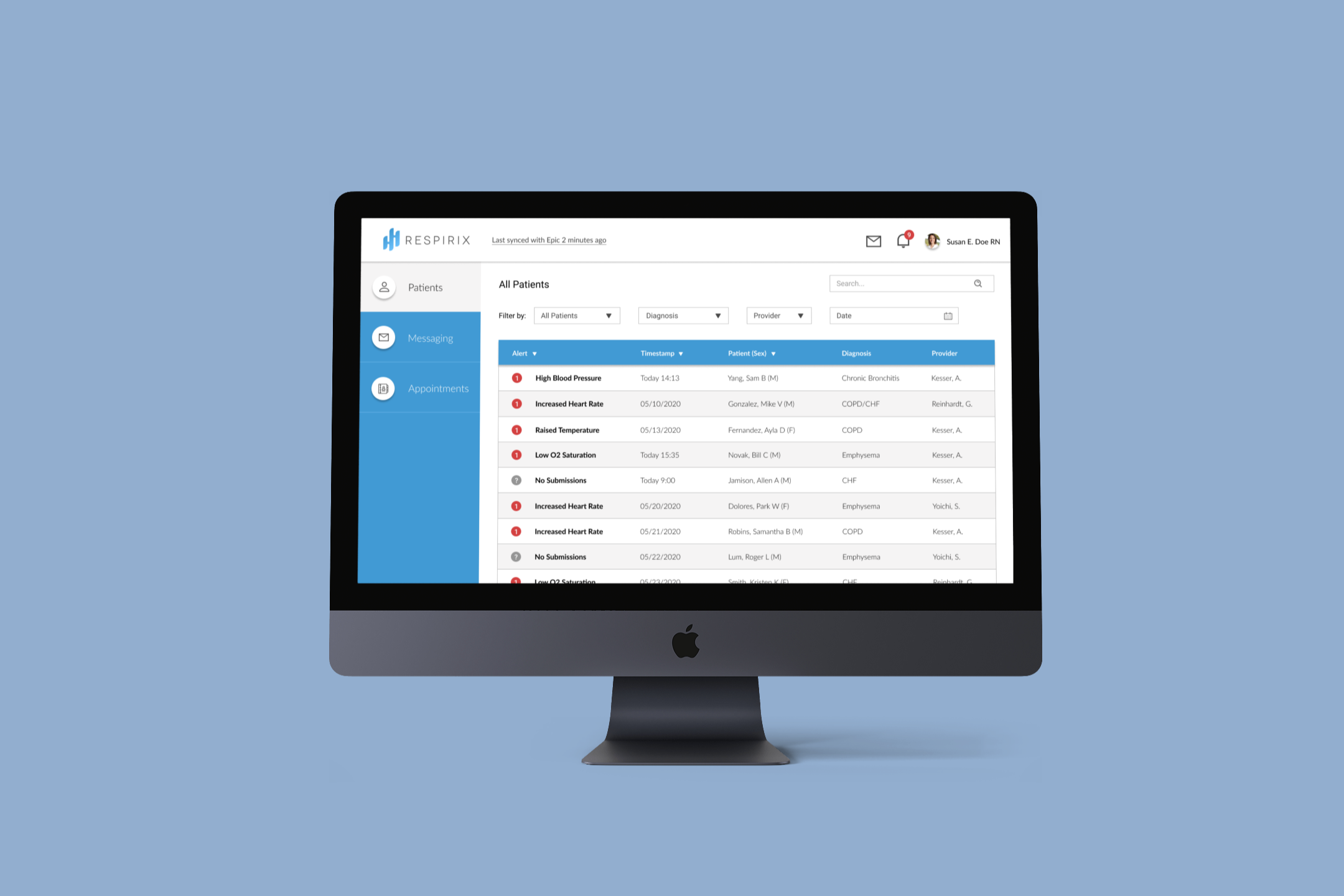
Clear and readable graphs and charts.
By presenting the collected data as easy-to-read graphs and charts, we save the users time and brainpower. The graphs make the data tangible, relevant, and actionable for the users.
Automated, tiered alerts.
Without automated alerts, our users would have to sift through thousands of charts daily, which is clearly unreasonable and a poor use of time. Based off our research, we created timestamped alerts that are distinguished and sorted by both alert type and alert severity.
Consistent patient data across all platforms.
As a medical practitioner, it is crucial to have the most up-to-date and comprehensive information about your patient. This is why we prioritized a continuous and reciprocal sync with the user’s EHR (electronic health record app). This action is automatic and instantaneous, and the user is able to see at all times when the patient data has last been synchronized with the EHR.
Video visits and in-app messaging.
We included a within system video call feature to ensure direct and efficient communication between the user and providers. This is also to help users assess the patients through direct observation.
Results and reflections.
Integration into Epic.
Epic is the most commonly used EHR in the field. It is inevitable for us to integrate the practitioner portal into Epic. Incorporating the app as an add-on to Epic will further streamline the user flow and reduce friction. Further iterations will be made in accordance with discussions with the software engineer team.
Analyze usage to validate core features.
One next step is to perform usage analytics with medical professionals. These will be used to assess time consumption on different sections of the portal. With this knowledge we can further improve the user interface to increase efficiency in usage.
Alert customization
It was very clear from our user interviews that no patient is alike. Each patient receives different care based on their health history and current condition. That’s why we believe it will be wise to include the ability to customize alert settings for each patient. There will be a default alert setting for all new patients, and the practitioner has the option to tailor the alert criteria for a specific patient.
Get in touch.
Let’s build something together.
jamesrothbart[at]gmail[dot]com
Oakland, San Francisco Bay Area